
One of the most common causes of back pain is osteochondrosis.According to statistics, around 80% of people suffer from this pathology.However, not all patients can accurately answer what osteochondrosis is.This is a chronic disease that affects the cartilage and bone tissue of the spine.Degenerative-dystrophic changes can affect any part of the spine or several at the same time.
To get rid of the disease faster, you should start treatment when the first signs of pathology appear.However, many people simply do not notice them and then the pathology develops and becomes more serious.
Osteochondrosis must be treated comprehensively: medications, physiotherapy, physiotherapy procedures, etc.If there are complications (intervertebral hernia, radiculitis, paralysis of the legs), surgery may be necessary.
What is it?
A chronic disease in which the intervertebral discs and bone tissue of the spine are damaged is called osteochondrosis.
The spine consists of 33 to 35 vertebrae, between which are cartilaginous pads (vertebral disc).They consist of a nucleus pulposus and an annulus fibrosus (outer portion);They are covered on both sides by dense and elastic vitreous hyaline cartilage.Thanks to the intervertebral discs, the spine becomes more elastic and mobile.
With osteochondrosis, metabolic processes and blood circulation in the spine are disturbed.Under the influence of negative factors, the discs between the vertebrae become less strong and elastic and their volume decreases.The spine contracts and the height of the cartilaginous pads decreases.
The gelatinous central part of the disc first swells and then dries out, then the depreciation of the spinal column is disturbed.The outer layer becomes thinner and cracks appear.When a gelatinous substance seeps there, bumps (bumps) form.When the outer part of the disc ruptures and the nucleus pulposus prolapses, an intervertebral hernia is diagnosed.
The disease osteochondrosis is manifested by discomfort, reduced mobility and pain in the affected area.When hernias appear, neurological alterations occur: back pain that extends to the upper or lower extremities, numbness of the arms, legs, groin, involuntary urination or defecation, etc.
Aid.Previously, osteochondrosis was diagnosed mainly in patients over 40 years of age.Now the disease is increasingly detected in younger people (16 to 30 years old).This is usually associated with a sedentary lifestyle.
Reasons
Degenerative-dystrophic changes in cartilage and bone tissue occur due to uneven loading on the elements of the spine.Then, in areas with excess pressure, the destruction of the intervertebral discs occurs.The pathological process can be caused by many negative factors.

The main causes of osteochondrosis:
- Injuries after a fall or blow.
- Congenital anomalies of the spine, genetic predisposition.
- Metabolic disorders due to poor nutrition, appearance of excess body weight.
- infectious diseases.
- Excessive stress on the spine during strength sports or heavy physical work.
- Chemical substances that enter the body through food or air.
- Frequent vibrations, for example from drivers.
- Flat feet.
- Wrong posture.
- Passive lifestyle, for example, among people with sedentary jobs (office workers, drivers).
- Smoking.
- Prolonged exposure to adverse weather conditions (low temperature and high humidity) on the body.
- Wearing anatomically incorrect shoes (tight or with heels).
- Frequent stress.
- Pregnancy, etc.
Often the disease manifests itself in people who carry a lot of weight on one hand, stay in the wrong position for a long time, or sleep on a too soft mattress or a high pillow.The likelihood of developing the disease increases with age-related changes associated with metabolic processes or blood supply to the vertebrae.This risk increases if a person frequently changes body position, bends, straightens, or shakes the body.
Reference.Osteochondrosis is often diagnosed in tall, stooped people with a weak muscle corset.And moving workers, professional athletes, builders and office workers are also at risk.
Types of osteochondrosis
As already mentioned, pathology can affect different parts of the spine.Depending on the location, the following types of osteochondrosis are distinguished:
- The lower back is the most common type of disease, since the load on the lumbosacral segment is quite high.The pathology is accompanied by pain in the lower back, which can spread to the legs, groin, and in the later stages, neurological disorders occur (impaired sensitivity of the lower part of the body).
- Cervical - also common.Degenerative-dystrophic changes are associated with weakness of the neck muscles, so even with minimal exposure there is a risk of vertebral displacement.It manifests itself as pain, which can radiate to the upper extremities, cephalalgia (headache), hearing and vision disorders.
- Thoracic is the rarest form of pathology.This is because the mobility of the thoracic segment is minimal;In addition, it is protected by the ribs, back and abdominal muscles.It is quite difficult to identify the disease, since its symptoms resemble those of other diseases.
And there is also osteochondrosis of several parts or of the entire spine at once.This type of disease has the most serious course.
Reference.According to medical statistics, osteochondrosis of the lumbar segment occurs in 50% of patients, cervical – 25%, thoracic – up to 10%.In 12% of cases, several parts of the spine are affected at once.
Classification of osteochondrosis according to its stage:
- Stage 1– the initial stage of pathology, which is manifested by dehydration of the nucleus pulposus, a decrease in the height of the cartilage pad and the appearance of cracks in its outer part.Diagnosing the disease at this stage is very difficult, since there are no obvious symptoms yet.The patient experiences slight discomfort in the damaged area if he remains in a certain position for a long time or actively moves.The pathology has a slow course, a latent form.It is discovered accidentally during an X-ray, MRI, or CT scan of the back.
- Stage 2– at this stage, the gap between the vertebrae decreases, the surrounding muscles and ligaments sag, and the likelihood of protrusions and displacement of the spinal elements increases.The cartilage lining begins to deteriorate, which is accompanied by pain.In the absence of adequate therapy, displaced discs or vertebrae can compress bundles of nerves, muscles and blood vessels.It is much easier to identify the disease at this stage.Complex conservative therapy is carried out.
- Stage 3– the outer part of the disc is destroyed, bulges and herniations form.In addition, the risk of subluxation increases and osteoarthritis of the intervertebral joints may develop.The patient experiences severe pain, which may extend to the upper or lower extremities, and sensitivity is impaired (tingling or numbness).
- Stage 4– due to excessive flexibility of the joints of the spine, bone growths appear in the contact areas, so the body tries to improve the fixation of neighboring vertebrae.Osteophytes often pinch nerve bundles and damage elements of the spine.Increases the risk of ankylosis, which leads to joint immobility.The patient develops severe pain, neurological disorders and difficulty moving.If left untreated, you can become disabled.
Osteochondrosis is a chronic disease that is important to detect in time to prevent dangerous complications.
Symptoms
The first signs of the disease are discomfort and a feeling of stiffness in the affected area.The patient's back tires faster and pain appears periodically.Then spinal osteochondrosis in adults is complemented by other symptoms.Clinical manifestations depend on the stage and location of the affected area.Therefore, patients need to know how the pathology of the cervical, thoracic and lumbar spine differs.This will allow you to notice warning signs in time and seek medical help.

Symptoms of spinal osteochondrosis, which affects the cervical spine:
- aching or stabbing pain that may spread to your upper back, neck, or arms;
- increased muscle tone around the affected area, which can be felt by palpation;
- headache, which intensifies during movement and is not relieved by analgesics;
- dizziness with sudden turns of the neck;
- visual impairment, which is manifested by “spots” or spots before the eyes;
- hearing disorders (noise or ringing in the ears);
- weakening of the neck or shoulder muscles;
- loss of sensation in the neck and hands;
- In rare cases, the patient's tongue becomes swollen and numb.
This type of pathology is most frequently observed in office workers.
Clinical manifestations of osteochondrosis of the lumbosacral segment:
- painful or sharp pain in the lower back;
- discomfort increases when the patient moves;
- pain syndrome can spread to the lower part of the body (buttocks, groin, legs);
- neurological disorders manifested as numbness, tingling, coldness in the groin, buttocks, legs;
- weakening, thinning of the leg muscles.
In some cases, due to severe pain, the patient cannot straighten his back, twist or bend.Try to adopt a position that relieves the discomfort.
Degenerative-dystrophic changes in the thoracic segment of the spine are accompanied by the following symptoms:
- periodic sharp pain in the chest, shoulder blades, which intensifies when raising the upper extremities or bending;
- the pain becomes more pronounced at night, after hypothermia, physical exertion;
- altered skin sensitivity;
- feeling of compression in the chest;
- During movement, a sharp pain may appear between the ribs.
Reference.Patients often confuse thoracic osteochondrosis with heart disease.However, during the first pathology, the pain intensifies with breathing and is not relieved by nitroglycerin.
When several parts of the spine are affected at once, specific symptoms appear.
Treatment methods
Once the doctor makes a diagnosis of osteochondrosis, treatment should begin.The treatment plan is drawn up by the doctor, taking into account the degree of the disease, its causes and the general condition of the patient.
During diagnosis, the following methods are used:
- Radiography.
- CT or MRI.
- Ultrasound of the spine.
- Myelography.
- Neurological tests.
Additionally, the patient may be prescribed laboratory tests.
Treatment of spinal osteochondrosis should be comprehensive.Depending on the severity, it lasts 4 to 8 weeks, then maintenance therapy is carried out for a long time (about a year).This will help consolidate the results and prevent relapses.
Your doctor will tell you what to do if you have osteochondrosis.Treatment usually begins with the use of conservative methods: taking medications, performing therapeutic exercises, physiotherapy, massage, etc.Surgical intervention is performed only in cases where the pain does not go away for a long time after drug treatment, there are neurological disorders, or the disease progresses rapidly.
Conservative methods will help eliminate pain and other unpleasant symptoms, normalize the functionality of the spine and avoid complications.
The drugs reduce the symptoms of the disease, improve blood supply and tissue trophism, and accelerate the healing of damaged areas.For this purpose, the following medications are used:
- Anti-inflammatory medications help relieve inflammation and pain.
- Antispasmodics help relax tense muscles and relieve pain.
- Preparations with antioxidant effects, for example, vitamin C, tocopherol, thioctic acid.
- To improve blood supply to the damaged area, vasodilators and vitamin B are used.
- To accelerate recovery or stop the further development of degenerative processes, chondroprotectors are used, preparations based on hyaluronic acid, glucosamine and chondroitin.
Reference.The fight against severe pain is carried out through therapeutic blocks.The medication is injected into the affected area.If steroids are added to local anesthetics, the therapeutic effect will last longer.This method of therapy is used if traditional methods (medications, rest, physical therapy) are ineffective.
The following conservative methods will help treat osteochondrosis:
- Physiotherapeutic procedures will help relieve pain and increase the effectiveness of medications.Additionally, they are used during the period of remission, when there are no serious symptoms.The most used treatments are ultrasound, laser treatment, magnetotherapy, diadynamic therapy, electrophoresis with the use of analgesics and anti-inflammatories.
- Therapeutic gymnastics helps to correct posture, strengthen the muscles of the back, abdomen, sides, ligaments, normalize muscle tone and relieve pain associated with compression of nerve bundles.Regular training will help improve blood circulation, nutrition of damaged spinal discs and accelerate their recovery.
- Kinesitherapy: safe exercises on special simulators.This technique allows you to relieve the axial load of the spine, restores microcirculation in the deep muscles, helps relieve pain, spasms, swelling, and normalizes the functionality of the damaged area.
Important.The doctor draws up a set of exercises for osteochondrosis for each patient individually.It is recommended to carry out the training under the supervision of an instructor.
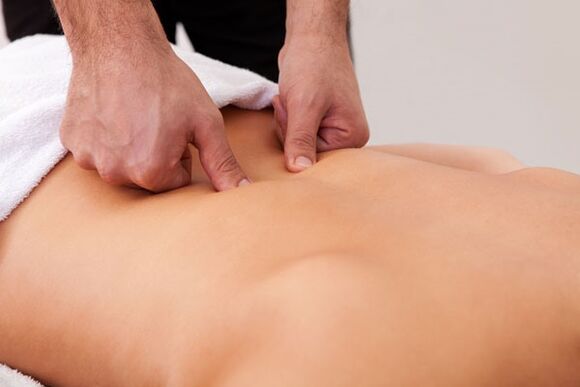
- Massage also helps to combat osteochondrosis as part of complex therapy.Therapeutic procedures improve blood flow to the spine, relax spasmodic muscles and improve tissue trophism.A very popular water body massage, which, in addition to the effects described above, normalizes the state of the nervous system.
- Manual therapy is the influence of the therapist's hands on the patient's body.Treatment methods are selected separately for each patient.After a course of treatment, blood circulation is normalized, metabolic processes in the damaged area are improved, its mobility is corrected, and the immune system is strengthened.Manual therapy helps prevent complications of osteochondrosis.The main thing is to find an experienced specialist.
- Traction is the stretching of the spine using special weights and simulators.The procedure helps eliminate vertebral displacement, increase intervertebral space and correct disorders of the spinal structure.
- Acupuncture - exposure to biologically active points on the body with fine sterilized needles.Acupuncture helps relax tight muscles and reduce pain.
To improve the condition, the patient is recommended to sleep on an orthopedic mattress.If your work involves sitting for a long time, then you need to purchase a chair with an orthopedic backrest, periodically get up and do back exercises.Additionally, stress and hypothermia should be avoided.
Chondrosis and osteochondrosis: what is the difference?
Chondrosis and osteochondrosis are related conditions.However, many patients do not understand the difference.
Chondrosis of the back is a disease that affects cartilage tissue.With osteochondrosis, degenerative-dystrophic changes spread to the vertebrae and surrounding tissues.This is the main difference between these two pathologies.That is, chondrosis is the first stage of osteochondrosis.
The causes of chondrosis and osteochondrosis are not different.However, they manifest themselves in different ways.
With chondrosis, cartilage tissue wears out, its composition changes or becomes thinner.For this reason, the intervertebral discs can no longer fully perform their shock absorption function.
Now you know the differences between chondrosis and osteochondrosis.
Symptoms of chondrosis
As already mentioned, identifying pathology at the first stage is very difficult, because it has a gradual course.Therefore, chondrosis is most often detected when bone tissue is affected, that is, osteochondrosis develops.
Spinal chondrosis is manifested by the following symptoms:
- increased back fatigue;
- incorrect posture;
- slight impairment of spinal mobility in the damaged area;
- Occasional mild back pain.
It is recommended to consult a doctor if you notice at least one manifestation of the disease.Then it will be possible to stop the process of cartilage destruction.
To identify chondrosis, it is recommended to perform an X-ray or MRI.This last study is more informative, since it allows you to notice the slightest changes in the structure of the cartilage.
Chondrosis treatment
To prevent chondrosis from turning into osteochondrosis, it is necessary to carry out complex treatment.For this, the patient is prescribed anti-inflammatory drugs, chondroprotectors and vitamins.Physiotherapy helps improve spinal mobility and strengthen muscles.The therapy can be complemented with physiotherapy procedures and reflexology.
Reviews
Most patients who started treatment of the disease on time are satisfied with the results of therapy.The pain and stiffness in my spine disappeared.But to achieve such results it is necessary to carry out a wide range of measures.
- Man, 38 years old: "I was diagnosed with lumbar osteochondrosis in the second stage. The doctor prescribed injections for a month and a half and 10 massage sessions. In addition, he began to perform therapeutic exercises. After the course the pain disappeared. I will repeat the course in a month to consolidate the results."
- Woman, 45 years old: "I couldn't straighten up due to pain due to osteochondrosis. The doctor prescribed injections, massage and magnetic therapy. In addition, I tried to do exercises every day and took chondroprotectors. After completing the treatment, the pain disappeared."
- Woman, 44 years old: "I have cervical osteochondrosis, which I managed to get rid of twice. She provided me with complex treatment: medications, physiotherapy, massage, exercise therapy, swimming pool. But 3 years after the last treatment, severe pain and numbness appeared in the neck, shoulder blade and arm. I went to the doctor and an MRI revealed a hernia. I was referred to a neurosurgeon who scheduled surgery. After removing the protrusion, sheHe underwent rehab. It's been a year now and nothing bothers me yet.”
The most important thing
Osteochondrosis is an insidious disease that is difficult to detect in stage 1 and can be confused with other pathologies.It is better to visit a doctor when the first signs of the disease appear (discomfort, stiffness in the damaged area), then it will be easier to cure it.It is important to carry out complex therapy: medications, physiotherapy, massage, physiotherapy, manual therapy, etc.If conservative methods do not help for more than 6 months, there are neurological disorders or other serious complications, then surgery cannot be avoided.


















